ReachMD
Be part of the knowledge.™Patient-Led Intervention First to Address Difficult Dialysis Symptoms
6/20/2023
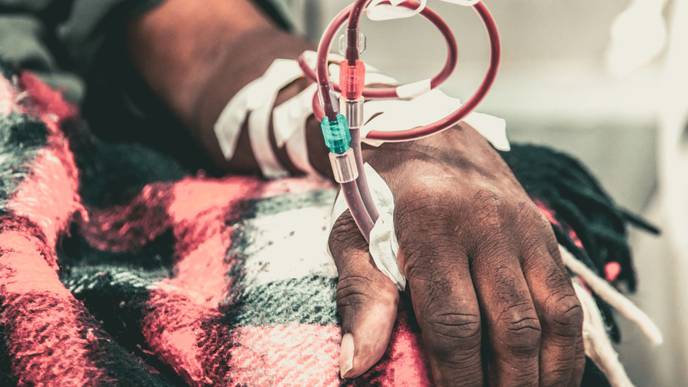
PITTSBURGH — When a patient with chronic kidney disease finally reaches the point that their kidneys fail, doctors have a treatment available: dialysis. But undergoing dialysis often brings a high burden of other unpleasant symptoms — fatigue, pain and depression — that are outside the typical nephrologist’s wheelhouse and can be difficult to treat.
A new patient-guided intervention using telemedicine improves these troublesome symptoms with results that persist for several months after the intervention ends, according to the results of a randomized clinical trial published today in JAMA Internal Medicine by physician-scientists at the University of Pittsburgh and University of New Mexico.
“Our patients and their caregivers report pain, fatigue and depression as major issues related to dialysis that affect their participation in life,” said lead author Manisha Jhamb, M.D., M.P.H., associate professor in the Pitt School of Medicine’s Renal-Electrolyte Division. “It’s the nephrology community’s responsibility to study interventions that address patients’ mental health and quality of life concerns; otherwise, we are failing our patients. This study is a step in that direction.”
Nearly half a million people in the U.S. with end-stage kidney disease — when the kidneys stop functioning — receive dialysis, where they are hooked to a machine at least three days a week for several hours to filter waste and extra fluid from their blood. At a recent National Institutes of Health workshop, patient stakeholders emphasized that post-dialysis fatigue is a serious concern.
“Dialysis is a life-saving treatment, but it’s a huge burden and a major life change for patients and their families,” Jhamb said. “Many people are unable to work or enjoy life because of the demands of the treatment and the way it affects their physical and mental health.”
Jhamb and her colleagues developed the Technology Assisted Stepped Collaborative Care (TĀCcare) trial to test whether 12 weekly sessions of cognitive behavioral therapy delivered via telemedicine either while patients receive their dialysis or at home could improve symptoms. To ensure the results weren’t simply an effect of the added attention from the tele-sessions, they had a comparison group of patients receive weekly health education via telemedicine.
Jhamb partnered with senior author Mark Unruh, M.D., M.S., professor in the University of New Mexico School of Medicine’s Division of Nephrology, to recruit a diverse pool of 160 participants from Pennsylvania and New Mexico who were receiving dialysis and had clinically significant levels of fatigue, pain or depression. They averaged 58 years old, and 28% were Black, 13% American Indian and 18% Hispanic.
The intervention allows the patient to set goals and tailor the care to address their specific concerns. For example, if the patient is concerned about pain, they can focus on psychotherapies to manage that pain and also receive medications.
“It was initially surprising that very few participants wanted medication for their symptoms — they were much more focused on the behavioral therapy,” Jhamb said. “But when you think about it, it makes sense: These patients are taking 10 or more medications per day. They don’t want another pill.”
Compared to those who received educational materials, patients who received TĀCcare had a 6% improvement in energy levels and a 10% improvement in pain severity, both of which were sustained for six months following therapy. They also had an improvement in depression symptoms, but it was very small, something Jhamb partially attributes to only a small number of participants initially having clinically significant depression.
“These results are really promising and in the range seen by similar interventions for cancer patients,” said Jhamb. “Until now, analgesic medications for pain and recommendations for better sleep and exercise to address fatigue have been the main suggestions we’ve been able to offer our patients, and they haven’t been satisfactory.”
The diversity of study participants also indicates that the results are generalizable to broad populations. Additionally, the successful use of telemedicine with rural participants in New Mexico provides an opportunity to offer TĀCcare to patients who might otherwise not have access to these specialized behavioral therapy services.
Jhamb says the next steps involve a cost-benefit analysis so that policymakers and insurers can consider mandating and paying for the intervention, as well as trials to test if “booster” sessions could prolong the results beyond six months.
Additional authors on this research are Jennifer L. Steel, Ph.D., Jonathan G. Yabes, Ph.D., Susan M. Devaraj, Ph.D., Yoram Vodovotz, Ph.D., Scott Beach, Ph.D., Steven D. Weisbord, M.D., M.Sc., and Bruce Rollman, M.D., M.P.H., all of Pitt; Maria-Eleni Roumelioti, M.D., and Sarah Erickson, Ph.D., both of the University of New Mexico; and Kevin E. Vowles, Ph.D., of the University of Belfast in the U.K.
This research was supported by National Institutes of Health grant R01DK114085.
PHOTO DETAILS: (click image for high-res version)
CREDIT: UPMC
CAPTION: Manisha Jhamb, M.D., M.P.H.
Facebook Comments