ReachMD
Be part of the knowledge.™New Practice-Changing Research Links ARD to Bacteria
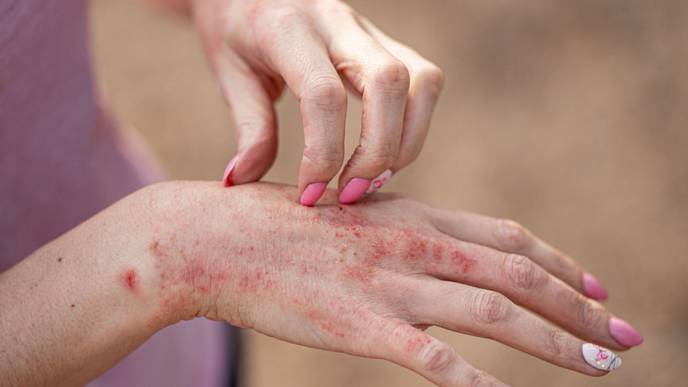
As many as 95% of people undergoing radiation treatment for cancer will develop acute radiation dermatitis (ARD). Little, however, has been known about why this condition occurs, and there are no widely adapted or standardized treatments for preventing severe ARD.
New research may change all of this.
Many cases of ARD involve Staphylococcus aureus, and simple, low-cost treatment may prevent severe cases, potentially setting a new standard of care for people undergoing radiation therapy. The new protocol calls for patients to use a body cleanser such as chlorhexidine along with mupirocin 2% nasal ointment twice a day for 5 days, every other week, throughout their radiation treatment.
These findings were reported in two articles published in JAMA Oncology.
Study author Beth N. McLellan, MD, director of supportive oncodermatology at Montefiore Einstein Cancer Center and chief of the division of dermatology at Montefiore Health System and Albert Einstein College of Medicine in the Bronx, New York, discussed the findings with DermWire.
For the study, Dr. McLellan and colleagues enrolled 76 patients undergoing radiation therapy for cancer. The investigators collected bacterial cultures from patients before and after radiation treatment from inside the nose, the skin in the radiated area, and skin on the side of the body not exposed to radiation. Before treatment, approximately 20% of patients tested positive for S aureus bacteria but did not have an active infection. Following treatment, 48% of patients who developed severe ARD tested positive for the presence of S aureus bacteria compared with only 17% of patients who developed the mildest form of the condition. Many patients with S aureus on their skin also tested positive for nasal S aureus, suggesting that the bacteria from the nose might be infecting the skin.
The second study enrolled 77 patients undergoing radiation therapy. Participants were randomly assigned to receive either the standard of care (normal hygiene and moisturizing treatment such as Aquaphor) or the experimental antibacterial regimen. Although more than half of the patients treated with the antibacterial regimen developed mild to moderate ARD, no patient developed moist desquamation or experienced adverse effects from the treatment. In contrast, severe ARD affected 23% of participants receiving the standard of care, the study showed.
What do these findings add to the literature?
Beth N. McLellan, MD: “Until now, ARD was assumed to result simply from the skin being burned by the radiation, which meant that not much could be done to prevent it, but we show one of the most successful interventions for radiation dermatitis to date, which is a safe and easy topical regimen that addresses harmful bacteria on the skin."
How may bacteria cause or worsen ARD?
Dr. McLellan: “Radiation causes damage to skin cells leading to inflammation. Anytime the skin barrier is compromised, harmful bacteria can enter the skin and lead to more inflammation and sometimes infection. Radiation weakens the skin’s structure at the treatment site and can result in infection by allowing S aureus bacteria to break through the skin’s outer layer. Courses of radiation therapy—routinely requiring daily treatments over several weeks—increase the risk for skin infection to occur."
How will this affect treatment and prevention?
Dr. McLellan: “The readily available treatment we’ve developed and clinically tested could potentially save hundreds of thousands of people each year in the United States from severe ARD and its excruciating side effects. We hope that this regimen can be implemented for prevention of radiation dermatitis in people with breast cancer and that more studies will be done to examine the effects in other cancer types. I expect this will completely change protocols for people undergoing radiation therapy for breast cancer. A majority of participants in the studies were Black and Hispanic, suggesting that this protocol is generalizable and effective for people of different races and ethnicities. This is especially important because people with darker skin types are more likely to develop severe ARD.”
How does ARD affect the quality of life of patients with cancer?
Dr. McLellan: “ARD can significantly decrease people’s quality of life. It can cause pain, burning, and itching, which can disrupt sleep and affect what types of clothes people can wear. It can cause significant darkening of the skin and, long term, can lead to hardening of the skin called fibrosis. Our work is always motivated by a desire to help people with cancer receive the most effective treatment with the least amount of distressing side effects. We think we’ve done that here.”
Facebook Comments