ReachMD
Be part of the knowledge.™Metabolite in Urine Predicts Diabetic Kidney Failure 5-10 Years Early; Oral Therapeutic Drug Shows Promise in Mice
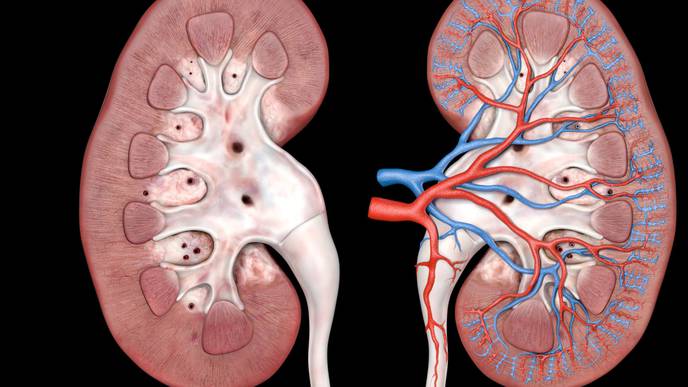
Current leading marker, protein in urine, does not apply to all patients with diabetes who develop kidney disease
Contact: Will Sansom, 210-567-2579, sansom@uthscsa.edu
SAN ANTONIO (Aug. 24, 2023) — Urine levels of adenine, a metabolite produced in the kidney, are predictive and a causative biomarker of looming progressive kidney failure in patients with diabetes, a finding that could lead to earlier diagnosis and intervention, researchers from The University of Texas Health Science Center at San Antonio (also called UT Health San Antonio) reported Aug. 24 in the Journal of Clinical Investigation.
Elevated adenine was also associated with all-cause mortality.
The study results are significant because until now, the most important marker for kidney disease has been protein (or albumin) in the urine. Up to half of diabetes patients who develop kidney failure never have much protein in their urine. As 90% of patients with diabetes (more than 37 million patients in the U.S.) remain at increased risk despite low levels of albumin in their urine, this study has widespread consequences. It is the first study to identify these patients at an early stage by measuring this new causative marker in the urine.
The finding paves the way for clinic testing to determine — five to 10 years before kidney failure — that a patient is at risk, said the senior study author, Kumar Sharma, MD. Sharma is professor and chief of nephrology at UT Health San Antonio, where he is the founding director of the Center for Precision Medicine. He is also vice chairman for research in the Department of Medicine in the Joe R. and Teresa Lozano Long School of Medicine.
Importantly, the research team identified a small molecule that blocks the major pathway of endogenous adenine production in the body. This therapeutic drug reduced kidney adenine levels in mice with type 2 diabetes. “The drug protected against all the major aspects of diabetic kidney disease without affecting blood sugar,” Sharma said. “The study is remarkable as it could pave the way to precision medicine for diabetic kidney disease at an early stage of the disease.”
Findings consistent across diverse study populations
The researchers studied more than 1,200 patients with diabetes across three international research cohorts. The Chronic Renal Insufficiency Cohort (CRIC) study included African American, Hispanic and Caucasian participants in the U.S. A separate study was in the American Indian population. The team also evaluated an Asian cohort of mostly Chinese, Asian Indians and Malay populations in a study based in Singapore.
“In each study there was the same pattern, that high urine adenine was associated with higher risk of kidney failure,” Sharma said. “We are truly grateful for all the participants in this global study, and I would like to thank all of the investigators and research teams who were part of this collaborative effort.”
Mapping the metabolites
UT Health San Antonio is one of a few centers in the U.S. perfecting a technique called spatial metabolomics on kidney biopsies from human patients. This technique enables researchers to determine the locations of adenine and other small molecules in kidney tissues. The kidney biopsies were provided from academic centers throughout the United States as part of the Kidney Precision Medicine Project, a national collaborative and innovative program supported by the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
“It’s a very difficult technique, and it took us several years to develop a method where we combine high resolution of the geography of the kidney with mass spectrometry analysis to look at the metabolites,” Sharma said.
Metabolites are small molecules that the body produces based on metabolism. They make cells go in a healthy way or in a disease pattern, Sharma said.
Adenine situated around kidney blood vessels
The team found endogenous adenine around scarred blood vessels in the kidney and around tubular-shaped kidney cells that were being destroyed. Endogenous substances are those that naturally occur in the body.
The finding that high levels of adenine were also associated with all-cause mortality in the study participants suggests that the metabolite is affecting other parts of the body, as well, Sharma said.
False sense of security
Many patients with diabetes know they’re at risk of kidney disease, but if they don’t have protein in their urine, they think they are protected, he said.
“They could be feeling a false sense of security that there is no kidney disease occurring in their body,” Sharma said. “But in fact, in many cases it is progressing, and they often don’t find out until the kidney disease is pretty far advanced. And at that time, it is much harder to protect the kidneys and prevent dialysis.”
Life-altering treatment
Once a patient needs dialysis, he or she must have a fistula or catheter placed and go on a dialysis machine three times a week, four hours at a time to clean the blood.
“The death rate is very high, especially in patients with diabetes,” Sharma said. “There is about 40% mortality within five years in patients with diabetes and kidney failure.”
A new type of therapy is needed
Although treatments to protect against diabetes and blood pressure are improving, they only push the envelope a little bit, Sharma said, in that patients still have progressive kidney disease and kidney failure, but they are afforded more time before they reach that endpoint. The measurement of urine adenine is difficult; however, the team at the Center for Precision Medicine at UT Health San Antonio has developed a robust and sensitive method to measure urine adenine in patients.
“What we’re hoping is that by identifying patients early in their course and with new therapies targeting adenine and kidney scarring, we can block kidney disease or extend the life of the kidney much longer,” Sharma said.
Acknowledgments
This research is made possible by funding from the National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases, grant numbers UO1DK114920 and UH3DK114920.
Endogenous adenine mediates kidney injury in diabetic models and predicts diabetic kidney disease in patients
Kumar Sharma, MD; Guanshi Zhang, PhD; Jens Hansen, MD; Petter Bjornstad, MD; Hak Joo Lee, PhD; Rajasree Menon, PhD; Leila Hejazi, PhD; Jian-Jun Liu, MBBS; Anthony Franzone, BS; Helen C. Looker, MBBS; Byeong Yeob Choi, PhD; Roman Fernandez, MS; Manjeri A. Venkatachalam, MBBS; Luxcia Kugathasan, BSc; Vikas S. Sridhar, MD; Loki Natarajan, PhD; Jing Zhang, MS; Varun Sharma, MSc; Brian Kwan, PhD; Sushrut Waikar, MD; Jonathan Himmelfarb, MD; Katherine Tuttle, MD; Bryan Kestenbaum, MD; Tobias Fuhrer, PhD; Harold Feldman, MD; Ian H. de Boer, MD; Fabio C. Tucci, PhD; John Sedor, MD; Hiddo Lambers Heerspink, PhD; Jennifer Schaub, MD; Edgar Otto, PhD; Jeffrey B. Hodgin, MD; Matthias Kretzler, MD; Christopher Anderton, PhD; Theodore Alexandrov, PhD; David Cherney, MD; Su Chi Lim, MBBS; Robert G. Nelson MD; Jonathan Gelfond, MD; Ravi Iyengar, PhD, for the Kidney Precision Medicine Project
First published: Aug. 24, 2023, Journal of Clinical Investigation
https://www.jci.org/articles/view/170341
The University of Texas Health Science Center at San Antonio (UT Health San Antonio) is one of the country’s leading health science universities and is designated as a Hispanic-Serving Institution by the U.S. Department of Education. With missions of teaching, research, patient care and community engagement, its schools of medicine, nursing, dentistry, health professions, graduate biomedical sciences and public health have graduated more than 42,300 alumni who are leading change, advancing their fields and renewing hope for patients and their families throughout South Texas and the world. To learn about the many ways “We make lives better®,” visit UTHealthSA.org.
Stay connected with The University of Texas Health Science Center at San Antonio on Facebook, Twitter, LinkedIn, Instagram and YouTube.
Facebook Comments