ReachMD
Be part of the knowledge.™Leprosy Cases Rise in Florida: What Do Dermatologists Need to Know?
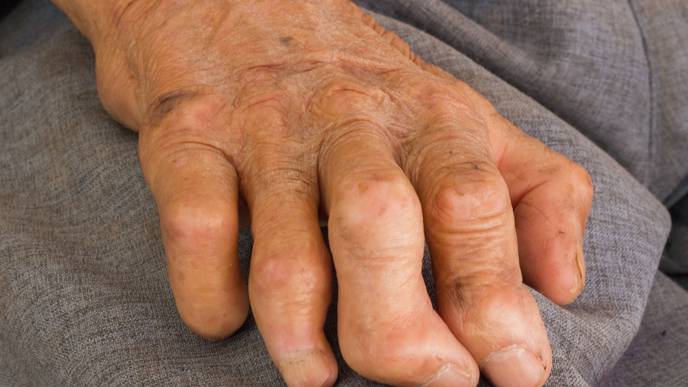
Leprosy is making headlines due to an outbreak in Florida, and while this disease is still rare, it should be on dermatologist’s radar, says Carrie Kovarik, MD, a professor of dermatology and medicine at Perelman School of Medicine at the University of Pennsylvania in Philadelphia.
Leprosy is still uncommon in the US, with an average of 180 cases/year reported in the US between 2011-2020, but there has been a change in the geography and epidemiology of the cases over the last decade. The number of reported cases has more than doubled in the southeastern states over the last decade, with a large proportion coming from Central Florida, according to the National Hanson’s (Leprosy) Disease Program. The Centers for Disease Control and Prevention reports that the growing body of literature suggests that central Florida represents an endemic location for leprosy.
“Historically, the majority of patients in the US with leprosy lived or worked outside the country in disease-endemic areas and acquired their disease abroad or had prolonged contact with immigrants from leprosy-endemic countries; however, more recently, about 1/3 of people with leprosy in the US seem to have locally acquired the disease,” Dr. Kovarik tells DermWire.
The transmission mechanism for leprosy is not entirely known although person-to-person transmission likely requires prolonged close contact. “Several research studies have also shown that a high proportion of cases in the southeastern US, with no known traditional risk factors for leprosy, carry the same unique strain as nine-banded armadillos in the area.”
Although most of the patients do not report close contact with the armadillos, this suggests a role for zoonotic (animal to human) transmission, she says.
Armadillos that carry leprosy have long known to be present in Texas and Louisiana, but not until more recently were they found to be in other states, including Mississippi, Alabama, Georgia, and Florida. “It is difficult to predict if it will become more common in other locations,” she says.
Making a leprosy diagnosis in 2023
“Leprosy presents on a spectrum, from just 1-2 pink or light-colored patches on the skin, to 20 patches, or the entire skin being affected,” she says. Those affected can experience loss of sweating or numbness in the skin patches.
“A thorough history and physical exam should be done to evaluate for leprosy,” she says. “Skin biopsies should also be done.”
Biopsies should be collected with a 4–5 mm punch and specimens should be deep enough to include subcutaneous fat, and biopsies should also be taken from an active margin of a lesion if possible. “Several specimens should be taken if multiple morphologies exist,” she says. Moreover, a thorough neurologic exam should be done, as well as palpation for enlarged nerves.
“Fill out your pathology form thoroughly, in order to notify your dermatopathologist of your suspicion, so that the appropriate stains can be ordered,” she says. “In difficult cases, the National Hanson’ Disease (Leprosy) Program can perform PCR on formalin-fixed, paraffin-embedded tissue or can perform secondary pathology review.”
When leprosy presents as a progressed disease, complications can occur, including involvement of the eyes and mucous membranes, she says.
The good news is that darly treatment of early disease gives an excellent prognosis and helps to prevent complications.
“Dapsone, rifampin, and clofazimine (in multibacillary cases) are the standard medications that are used for treatment,’ she says. Treatment lasts 1-2 years, depending on the type of leprosy and includes laboratory monitoring.
Facebook Comments