ReachMD
Be part of the knowledge.™AI Can Detect Breast Cancer as Well as Radiologists, Study Finds
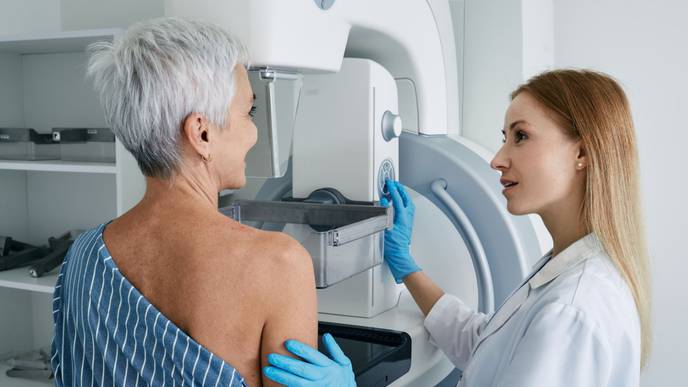
Artificial intelligence can detect breast cancer in mammograms as effectively as experienced radiologists, according to a new study that some experts are calling a game changer for the field of oncology.The emerging technology could cut radiologists’ workload by about half, freeing them for more advanced diagnostic work, the study found.
The preliminary analysis of a long-term trial of 80,000 women in Sweden, published Tuesday in the journal Lancet Oncology, showed that AI readings of mammograms actually detected 20 percent more cases of breast cancer than the “standard” reading by two radiologists. The AI assessments were verified by one or two radiologists, depending on the patient’s risk profile.
This led the researchers to conclude that using AI in mammography screening is a “safe” way tohelp cut patient waiting times and reduce the pressure on radiologists amid a global workforce shortage.
It may be a while beforemammograms will be read by a machine — as the authors and other experts have warned that AI models need to be trained and tested more before they can be deployed in health-care settings.
Still, the findings are “breathtaking,” wrote Nereo Segnan and Antonio Ponti, experts affiliated with the Center for Epidemiology and Cancer Prevention in Turin, Italy, who were not involved in the analysis.
In an article accompanying the release of the study, they suggest that integrating AI in screening procedures could ultimately “reduce breast cancer mortality” by making sure breast cancer is identified sooner, when it is more treatable. This would bea huge win, given that breast cancer is the “world’s most prevalent cancer,” according to the World Health Organization.
The analysis is “game changing,” Robert O’Connor, director of Ireland’s National Clinical Trials Office (NCTO), wrote on X, formerly known as Twitter. Itshows that AI could help triage mammograms according to cancer risk and identify breast cancer in those mammograms at a higher rate than radiologists with at least a couple of years of experience.
Using machine learning to try to improve medical diagnostics is not new, but it has accelerated in recent years with advancements in artificial intelligence.
The findings from this study are in line with emerging research showing that AI could help humans identify cancer earlier or more accurately, possibly leading to better outcomes for patients. The study is the first randomized controlled trial to investigate the use of AI in mammography screening, according to its authors.
The trial recruited 80,020 women from 40 to 80 years old who had mammographies in Sweden between April 2021 and July 2022. Half of them were randomly assigned to have their mammograms read by a commercially available AI model and by one or two radiologists, depending on the risk score on a scale of 1 to 10 that the AI assigned them in an initial screening. The other half had their mammograms assessed by two radiologists, the “standard” in Europe, according to the authors.
The AI model also supplied radiologists with information from the initial screening designed to help them accurately interpret mammograms. If the mammograms were flagged as suspicious, women were asked to come back for more tests.
In total, AI-supported screenings detected breast cancer in 244 women, compared to 203 in the standard screening group — a difference of 20 percent.
Improving the rates at which breast cancers are caught is crucial because early-stage breast cancers are increasingly treatable.
The disease killed at least 685,000 women worldwide in 2020, according to the WHO. In the United States, the average woman has a 13 percent chance of developing breast cancer in her lifetime — and a roughly 2.5 percent chance of dying of the disease, the American Cancer Society says.
In the study, AI-supported screenings didn’t lead to higher rates of false positives.
The authors didn’t measure the time it took radiologists to do the readings, but assuming a rate of about 50 readings per hour per radiologist, they calculated that it would have taken one radiologist 4 to 6 months less to read the mammograms in the AI test group compared to the mammograms in the standard screening group.
James O’Connor, a professor of radiology at the Institute of Cancer Research in London, said that integrating AI into breast cancer screenings could have a huge impact on the day-to-day work of people in his field.
If AI-supported screenings could be implemented “across different jurisdictions [and] populations,” and be “accepted by patients and by regulators as well as health-care professionals, then this does have the potential to save a lot of time, and this could help with shortages in workflow,” he said. But questions remain around implementation, he said, particularly because countries have different regulations regarding AI diagnostics, and some patients may not agree to the use of AI in the course of their medical care.
James O’Connor said the idea that artificial intelligence would ever replace radiologists is “nonsense.” In the hospital where he works, as well as many others around the world, there is a shortage of experienced radiologists and an increasing pile of scans to be read. Instead, he says that the right AI model, if well-implemented, could help radiologists focus on tougher cases to diagnose and on other types of scans.
“Usually, if you can replace something with AI, it was probably not the best use of human time anyway,” he said.
Kristina Lang, the lead author of the study, said in a news release that the interim safety results are “promising” but “not enough on their own to confirm that AI is ready to be implemented in mammography screening.”
One concern arising from the study is that, in detecting more cancers, the AI-supported screening may also over-diagnose or catch cancers that represent a low risk to patients.
In the study, screenings done with the help of AI detected more “in situ” cancers — cancerous cells that haven’t yet spread and may turn out to be low-grade. As the authors point out, this could lead patients and doctors to over-treat something that isn’t necessarily a threat — including through mastectomies, or the surgical removal of one or both breasts.
Another limitation of the study is that it did not collect data on the race and ethnicity of patients, so it cannot determine if the AI-supported screenings are better at identifying cancers in particular groups over others.
“Breast cancer can present slightly differently in [different] ethnicities & at different ages so validation in more countries will be vital,” wrote the NCTO’s Robert O’Connor.
Facebook Comments